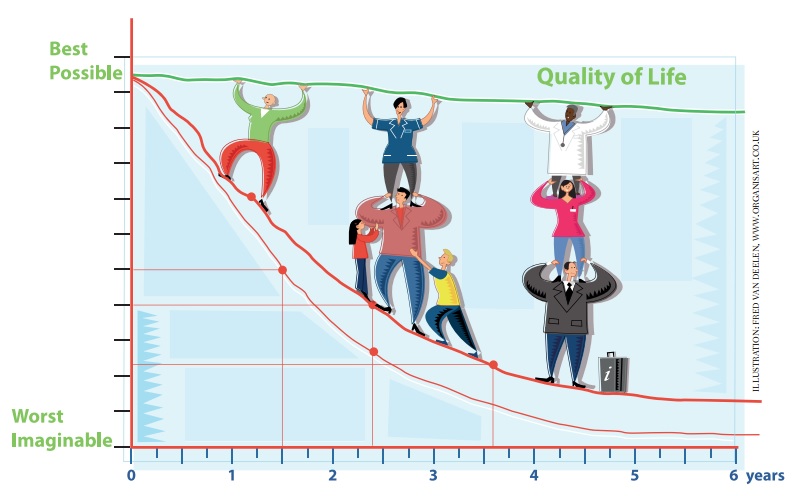
Sustaining a good quality of life becomes harder as cancers progress. Advocates are saying their needs have gone unmet for too long, and are working with professionals to define what they need and how best to access it.
Quality of life is important to everyone with an illness, but for those with advanced cancer there is a particular spectrum of needs that affect wellbeing – some of which are more ‘unmet’ than others.
Some of these relate to healthcare, such as managing the symptoms of the cancer, the side-effects of the treatment, and anxiety and depression. But people with advanced cancer also have other needs, which include effective communications with health professionals, emotional support from family and friends, and practical support to enable them, for instance, to stay working, access insurance, or get help with financial hardship.
Women (and some men) with advanced breast cancer comprise one of the largest groups to face these issues, and they are the focus of the Advanced Breast Cancer consensus conference, now coming up to its third event (ABC3), in Lisbon in November. A group of experts – who include patient advocates – draw up consensus guidelines following the conference, and they recognise that quality of life is fundamental to people with advanced disease, because it is one of the main aims of treatment.
While the population living for many years with metastatic breast cancer is growing, owing to a variety of new drugs, median survival has remained at about two to three years for some time. Around 40% of people with locally advanced (stage 3) disease die within five years.
During much of this time, women are likely to be undergoing various treatments, and there is an “implicit assumption”, the ABC guidelines say, that recording of adverse events by clinicians reliably documents patients’ side-effects and symptoms. “However,” they add, “there is an accumulating body of evidence suggesting that the frequency and severity of many symptoms that impact on an individual patient’s quality of life go under-reported, under-recognised, and consequently undertreated.”
Since the advent of chemotherapy, research groups have developed various instruments that aim to capture quality of life measures in clinical trials, notably the European Organisation for the Research and Treatment of Cancer (EORTC), which pioneered such tools as far back as 1980.
Tumour-specific scales, such as for breast cancer, have been developed, and there is a growing interest in capturing the patient experience outside of clinical trials – mainly using various patient-reported outcomes (PRO) tools.
Musa Mayer, who runs the US-based patient advocacy site AdvancedBC.org, and is a member of the ABC consensus group, points out that much of the emphasis on quality of life has been on the health-related aspects of treatment. The ABC guidelines do also recommend providing comprehensive information, and state that, where possible, specialist cancer nurses (or preferably breast specialists) should be part of the team managing patients with advanced breast cancer, to offer wider support.
But as Mayer notes, it is harder to make more recommendations about other aspects of survivorship for an audience of global health professionals, given wide variations in societies and health systems. The discussion in the guidelines does emphasise, however, that as early as possible a multidisciplinary approach should encompass not only physical, but also functional, social, psychological and spiritual domains; that the disease context and the challenge of uncertainty should be discussed with patients and families; and certain needs should be supported such as social security, job flexibility, rehabilitation, body image (including sexuality), and home and childcare.
“Care should encompass not only physical, but also functional, social, psychological and spiritual domains”
“That briefly sums up the extent of possible unmet needs for advanced breast cancer patients that I have been expanding on in work for the Metastatic Breast Cancer Alliance in the US,” says Mayer. “What we have found is that, contrary to expectations, there have been a lot of studies that document many of the unmet needs and ways to solve them, but most of the work has been small scale and qualitative. But there are also a number of patient and advocate surveys, such as those supported by Novartis and Pfizer, that have added much information. To help describe the needs we have grouped quality of life into six categories – they do overlap but are relatively discrete.” (See panel below.)
Mayer highlights findings in these categories, starting with psychosocial distress, which the evidence suggests is widely prevalent among patients of all backgrounds. “But many patients are not being offered mental health services and this is leading to a lot of unnecessary suffering,” she says. “It can become particularly acute as the disease progresses and women are less able to carry out everyday activities that are critical to their well-being, but this is often when they are least able to ask for the help they need.”
Closely allied is emotional support, which Mayer feels especially strongly about. “My own experience with having breast cancer taught me that women with advanced disease suffer from much stigma and can often be made to feel unwelcome in support groups. Their needs and concerns are typically quite different. Peer support from other patients with advanced cancer is often helpful, as friends may withdraw, and it’s typical for emotional support to erode over time as the illness progresses.”
Making informed decisions about treatment depends on the quality of information and communication from health professionals. “Treatment choices are individualised and often complex, and because recurrence of breast cancer is rarely discussed by health professionals, many women don’t understand the difference between being diagnosed with early breast cancer and recurrent metastatic disease,” says Mayer. “After treatment for early breast cancer, it’s not unusual to want close surveillance and many unnecessary tests.”
Practical issues such as paying for care and access to insurance vary according to national policies. “Financial hardship is clearly one of the biggest issues in the US, but it also disproportionately affects the uninsured, minorities and those living in rural areas,” says Mayer. Issues such as getting time off work for treatment, arranging childcare or losing a job can arise anywhere.
And physical symptoms of having advanced breast cancer represent just one of the six dimensions. Mayer notes that people are often hesitant to ‘bother’ their oncologists about symptoms, wishing not to be seen as ‘complainers’. There can also be ambivalence about palliative care or more aggressive treatments during the disease course.
In the clinic
For many, quality of life will revolve around the cancer clinic, but what practically can be achieved currently at hospitals? Galina Velikova, professor of psychosocial and medical oncology at the Leeds Institute of Cancer and Pathology in the UK, has a long-standing interest in quality of life issues, having been concerned in the earlier days of chemotherapy about whether toxic drugs were actually benefiting patients. She has chaired the EORTC’s Quality of Life Group, and is also now President of the International Society of Quality of Life Research.
“Quality of life instruments, such as the EORTC’s, capture symptoms and side-effects, physical function and some psychosocial aspects and so are good starting points,” she says. “But they have been developed to assess drugs in clinical trials, and a big problem is that they may be too long and complicated to use in day-to-day clinical practice. There is also no agreement on which ones to use, and they can be out of date. For example, we are doing an update of the EORTC breast cancer module now because, as it was one of the first cancer-specific modules we did, it doesn’t take account of new systemic therapies and new surgical and radiotherapeutic techniques.”
“Quality of life tools may be too long and complicated to use in day-to-day clinical practice”
Her own work has included designing and validating self-report questionnaires for patients that can be used by clinicians to monitor people during drug therapy, and are most useful in helping to assess side-effects, which when controlled can allow people to function better (see www.pogweb.org). In breast cancer, most of this work is on chemotherapies delivered in the clinic, and Velikova says she’s hoping to get funding to do similar research on oral targeted drugs, where monitoring is harder to do as patients take them at home, away from hospital staff.
“It may be that this approach will guide us to use drugs with fewer side-effects,” she says, adding that an aim is also to integrate self-reports into electronic patient records to increase the potential for personalised treatment and research. This is difficult to achieve on a wider scale in large hospitals or health care organisations, and Velikova says that typically only ‘local champions’ will be able to swing support from hospital administrations to make this a standard for more integration.
Capturing and acting on psychological aspects is yet more difficult. “Oncologists and nurses are not good at diagnosing emotional distress and anxiety,” says Velikova, and in any case many patients don’t always want help and prefer to focus on their treatment, she adds. “We have done a trial where we screened patients for depression and anxiety and provided this information to clinicians. Although clinicians discussed emotional issues more frequently with those patients, the patients didn’t accept more referrals to psycho-oncology or other professional help. This seems to be true for those with mild and moderate symptoms, but there is no doubt we need to identify and refer those with severe depression.”
Mayer comments that there is stigma associated with mental health diagnoses and seeking help. “In the US this is a significant barrier. I agree though that medical professionals often don’t recognise treatable anxiety and depression and mistakenly think it ‘goes with the territory’ of advanced cancer.”
Velikova argues that cancer centre professionals, and in particular nurses, should be trained in communications skills for giving information and listening to concerns, and also to detect possible emotional distress.
This has been put forward, for example, in the UK guidelines for supportive and palliative care. “Clinical nurse specialists can engage in counselling and cognitive problem solving for low-level distress, and related to this we have had a programme in the UK on advanced communications skills funded by the National Cancer Action Team, but funding has tailed off now, which is a pity.”
Ideally, cancer centres should also have nurses who specialise in metastatic cancer, given that there is such a wide range of tumour types, treatments and disease trajectories. “Breast cancer can vary from aggressive in young women to indolent in older women, so there is a big need to provide the right care for each person,” says Velikova. “But even in our centre, which is quite large, we have only had one metastatic nurse specialist for about a year and a half now, and that’s only been possible through external funding from a charity.”
Looking at wider quality of life issues poses other problems, says Velikova. “When we measure something, it’s helpful to have a purpose – something we can do about it. But often we don’t have answers to hand. Good examples are sexual issues and body image in women with breast cancer – we just don’t have specialist services we can send them to. This is very different from factors where we have professionals to help, such as identifying and managing pain.”
“When we measure something, it’s helpful to have a purpose, but often we don’t have answers to hand”
This doesn’t mean that measuring wider quality of life issues isn’t important, at least to gauge the size of needs. “We have performed a large study on people living with advanced cancer [breast, ovarian, prostate, renal and colorectal]” says Velikova. “It’s a growing population in advanced breast cancer, because we have older patients living much longer with hormone-positive disease, and also young women with HER2-positive cancer, who are often treated with many lines of chemotherapy plus the targeted drugs. These patients know they are not being cured and are ‘sitting on a time bomb’, and they encounter new problems such as not being able to go on holiday because they can’t get insurance. Their psychological needs are not so much depression, but living with uncertainty and the fear of recurrence.”
Bringing this group and their needs to the attention of society is an important first step. But one major obstacle to providing better services for, and awareness of, women with advanced disease is simply that, in most countries, no one knows how many there are. Cancer registries tend to record the stage of cancer only at initial diagnosis, which in breast cancer in developed countries, is much more likely to be early-stage disease, so the many people who suffer from advanced metastatic disease are lost from those population statistics.
There has been a pilot in England to register metastatic breast cancer, but there have been no updates on the project lately. “Even with ten years of electronic records at Leeds we don’t have a good idea of metastatic disease numbers here,” comments Velikova.
So there is a broad range of unmet needs in advanced breast cancer, and one big challenge is that there is no one place where all can be met. Even within the acute healthcare setting there is much room for improvement in personalising both treatment and communications.
Healthcare systems need to do much more to identify how many people are living with chronic cancer and assess all their needs. These will include access to wider mental health services, community support (including advocacy groups, face to face and online) and specialist services. Changes are also needed within society at large, to better accommodate people living with cancer, to eliminate stigma and reduce the obstacles they face in their everyday life.
As Mayer concludes, none of these is insurmountable, as we already know from good practice and projects around the world. It is the aim of the advocates at ABC to give patient groups the evidence and the support to plug the gaps in a sustainable way for people living with advanced breast cancer, which could well help those with other types of advanced cancer too.
The six dimensions of quality of life
Six quality of life dimensions are set out in a paper on ‘Changing the Landscape for People Living with Metastatic Breast Cancer’, published by the Metastatic Alliance in the US, which has carried out a comprehensive distillation of the evidence:
- Addressing psychosocial distress – it is estimated that a third of patients suffer from mood disorders such as anxiety and major depression; the theme of loss is pervasive, such as loss of attractiveness and roles in family life; and many lack access to mental health services. But much can be done to equip people with adjustment and coping mechanisms, and to gain control over feelings of loss. Studies also show that better emotional function is linked to fewer physical symptoms.
- Emotional support – support from family, friends, advocacy groups and healthcare professionals can be crucial, as having advanced disease can lead to social withdrawal and stigma. While nearly all patients value emotional support, its desired form can vary greatly among individuals.
Information – access to high-quality information is a need for most patients, and seeking information is part of gaining control, but many also say information is hard to find and can be confusing. Different types and sources of information are needed throughout the disease course. - Communication and decision-making – this is a complex area as patients vary in the degree to which they want to take part in decision making, but many in any case do not receive guidance. Clear lines of communication at the end of life, while difficult for patients, families and healthcare providers, allows for better palliative care, and ensures that the patient’s wishes will be respected.
Relief of physical symptoms – fatigue is by far the most common symptom reported by patients and is often difficult to treat. Chronic pain is another common symptom, as are sleep problems. Communication difficulties about symptoms exist on both sides of the patient–professional relationship. - Practical issues – a majority of people with metastatic breast cancer are in the workforce at diagnosis, according to the Alliance’s sources, but within the first year about a half have quit or lost their jobs. Apart from financial hardship and navigating welfare systems, problems include managing the home, childcare, and transport.
Mapping the population and their needs
Apart from mainly small-scale research studies on quality of life, in recent years there have been a number of surveys that have done much to raise awareness of advanced breast cancer. They include the BRIDGE survey in 2009, a global survey conducted by Pfizer on 950 women in nine countries, and Count Us, Know Us, Join Us, and Here & Now, both led by Novartis, with Here & Now being a pan-European initiative.
Both Novartis and Pfizer will be releasing more research at the ABC conference. Novartis will be announcing the next stage in Here & Now, and a call to action. Pfizer is completing a major report and survey of patients, advocacy groups and cancer centres in a number of countries. Cancer World will have the highlights of these in our report on ABC3.